Oxycodone is a semi-synthetic opioid analgesic. Since 1917, when it was initially synthesised in Germany, it has been utilised in medical therapy. Following the prohibition of heroin in the United States, oxycodone was developed as a substitute pharmaceutical.
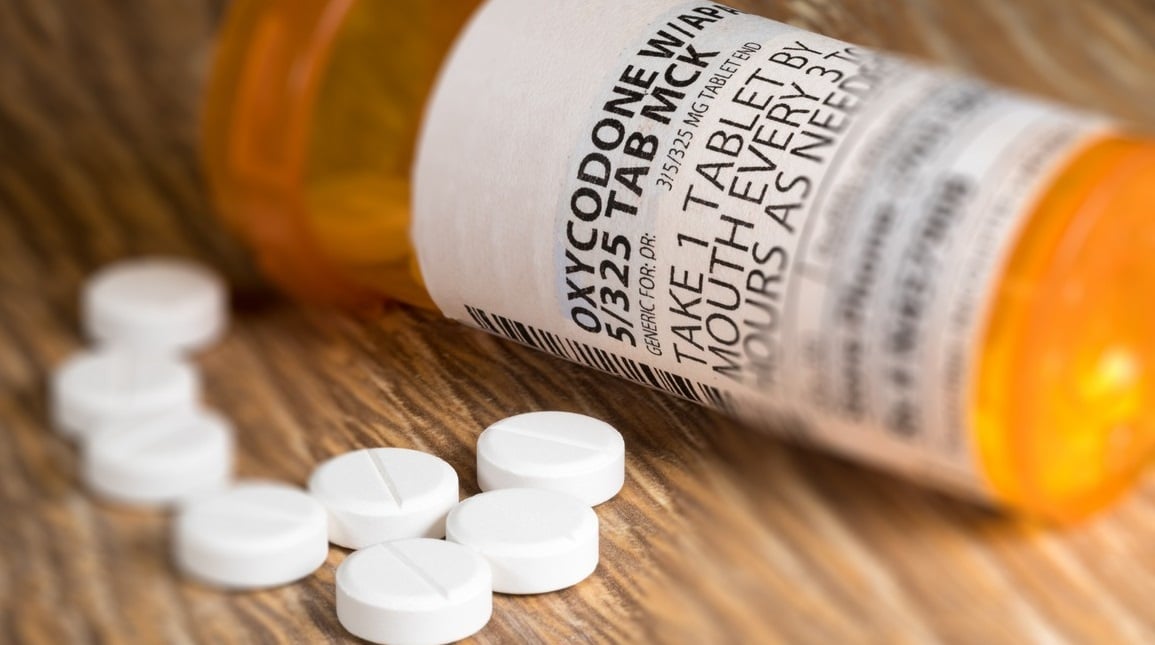
Oxycodone has always been a popular opioid, but after the emergence of Oxycontin, a medicine containing oxycodone, in 1996, its use in medical settings and for recreational purposes skyrocketed. It is becoming an increasing concern in the United Kingdom and many other countries. The German scientists that succeeded in synthesising oxycodone stated that it was not addictive.
The majority of opioid addiction disorders are caused by heroin. However, the number of conditions caused by prescribed opioids is growing. According to the World Health Organisation, around 275 million people took drugs at least once in 2016, with about 27 million suffering from an opioid use disorder. A nonfatal overdose occurs in about 45% of opioid addicts, while 70% see another person overdosing.
If your loved one needs support dealing with an Alcohol Addiction, contact us today on 0800 999 1083. We can help you by recommending treatment options.
In the United Kingdom, oxycodone is classified as a schedule 2 controlled substance. Prescriptions are kept track of, monitored, and recorded in a separate database. The entire quantity, number of doses, drug strength, and the correct legal name of the receiver must all be included in the prescription documentation. Patients must sign for their drugs at the pharmacy, and each prescription is suitable for 28 days.
Prescriptions for oxycodone or another schedule 2 drug may be picked up for people who cannot do so. The individual picking up the drug must provide identification, sign the prescription, and fill out any other documents that may be required. Most pharmacies usually require a letter of authorisation from the intended receiver.
Doctors and dentists can prescribe oxycodone, but doctors who prescribe opioids for addiction treatment need a Home Office licence. Oxycodone (OxyContin or another brand name for this opioid medication) is also prescribed by specially trained nurses for specific reasons, such as palliative care. Midwives have limited ability to prescribe pain medication during labour.
Oxycodone can be taken orally as a tablet, injected, given rectally (like an enema), or smoked.
On the market, there are dozens of oxycodone brands. Pure oxycodone, reformulations, and combination medicines containing both oxycodone and a non-addictive analgesic are all available.
A partial list of some of the other brand names is as follows:
Oxycodone is an opioid-receptor agonist that is semi-synthetic. It binds to opiate receptors in the brain, although it isn’t a naturally occurring phenanthrene alkaloid found in opium. The sap extracted from poppy heads is known as opium. The original alkaloids are codeine, morphine, and thebaine. Natural alkaloids’ molecular structures are changed to create synthetic opioids. Thebaine is the source of the majority of semi-synthetic opioids, including oxycodone.
The analgesic characteristics of oxycodone are similar to those of morphine. However, oxycodone has a longer half-life and higher bioavailability. Compared to morphine, oxycodone has fewer and milder adverse effects. Researchers believe that morphine has more severe side effects as a result of metabolites accumulating to dangerous levels. When medicine is metabolised, metabolites are the molecules created in the body. Oxycodone metabolism produces fewer metabolites than morphine metabolism.
Take OxyContin, for example, which takes effect after one hour on average and lasts for 12 hours. The drug activates two metabolites: oxymorphone, which is extremely powerful, and noroxycodone, which is rather weak.
Oxycodone is a pain reliever used to treat moderate to severe pain. It’s sometimes used as a short-term pain reliever after an injury or surgery and for chronic pain. It’s only used for persistent pain once non-opioid pain relievers have failed to work.
For patients who can’t take non-opioid pain relievers like NSAIDs or paracetamol, oxycodone is a choice. NSAIDs might worsen or induce ulcers and other gastrointestinal issues. People with liver disease or injury should avoid using paracetamol.
Extended-release oxycodone medicines should not be administered for acute pain or as a pain reliever. Extended-release oxycodone is used to treat persistent pain that requires continuous medication.
Oxycodone, like all opioids, loses its potency over time. Over time, pain alleviation and sensations of exhilaration, or ‘highs,’ diminish. After long-term use, everyone develops a physical reliance on opiates, but only some people develop an addiction.
Physical dependency is defined as the occurrence of withdrawal symptoms in the absence of the drug.
Addiction is defined as a persistent, ongoing psychological desire for oxycodone. Everything else in a person’s life can be overridden by compulsion. People who use the drug without following safety rules or doctor’s recommendations are at risk of becoming addicted. Substance users frequently believe they have control over their usage or that addiction ‘happens to others.’ In truth, only a small percentage of people can use opioids irresponsibly without experiencing issues.
Oxycodone is very addictive because it is derived from opiates. It binds to the same brain receptors that heroin does. The interaction with opiate receptors produces analgesia and a rush of dopamine, which causes euphoria.
A ‘high’ is a popular description of euphoria. Opioids alter the chemistry of the brain. Tolerance develops as a result of chemical changes in the brain, so the individual will require higher oxycodone doses to obtain the same effects.
Tolerance occurs when the brain and central nervous system become accustomed to a specific level of Oxycodone in the system. As a result of this issue, the drug is no longer as effective as it once was. The user must take additional Oxycodone to regain its previous effectiveness.
The first step toward physical dependency and addiction is to develop an Oxycodone tolerance. Tolerance can be treated early enough to avoid worsening an abuse problem. However, acquiring tolerance does not imply that a person is doomed to inescapable dependence.
Dependence is a state in which the brain and central nervous system have grown accustomed to Oxycodone to the point that they now rely on it to perform functions that they previously did without it. Some of the endorphins mentioned earlier, for example, aid in the normal regulation of pain. A person addicted to oxycodone may lose their ability to manufacture endorphins naturally. Oxycodone is used by the body to enhance endorphin production.
Addiction symptoms are determined by various factors, including a person’s living situation, economics, assets, and the intensity of the addiction. The following are six signs of opioid abuse:
Fatigue: Outside of normal sleep or nap times, the affected individual appears weary or tired on a regular basis.
Inability to perform to familiar standards: Drug addiction affects cognitive functioning and makes it difficult to concentrate. As a result, the person may find it challenging to meet the demands of family, job, or school. Missing work, failing to show up, leaving early, or demonstrating a significant reduction in performance are all possibilities.
Changes in lifestyle and personality: The individual may find it difficult to maintain family and interpersonal relationships due to drug usage. Individuals may withdraw from things that were once enjoyable, such as sports and other social activities. Individuals may experience social isolation due to their drug use, but they may also meet new people to consume drugs with.
Changes in appearance: In addition to displaying symptoms such as tiredness, the individual may become slack in their personal hygiene practices. As a result, a person may appear unkempt, wear filthy clothes, and cease purchasing or using grooming items.
Keeping a double life: People who abuse oxycodone often live a double life. Individuals who abuse oxycodone may employ code names or odd-sounding nicknames to allude to their drug use because it is an unlawful activity. Oxycodone is also known by the street names oxy, oxy cotton, oxy 80s, kickers, blue, killers, and hillbilly heroin.
Having drug-related paraphernalia: Different types of oxycodone abuse can influence the paraphernalia hidden in an individual’s home environment.
People who smoke oxycodone need a mortar and pestle-style crushing equipment, a pipe or pipe-like object to inhale the smoke, and a heat source, such as a lighter, at the very least. Individuals frequently use small pieces of metal to heat up the medication. These aluminium pieces can be thrown out or rolled up and strewn around. They will reveal burn stripes when unfurled.
A syringe, an instrument of some sort to cook the oxycodone in, a heat source, and a rope or belt would be included in oxycodone injection paraphernalia (to tie to the arm and make it easier to find a vein).
An enema or suppository, or something similar, will be required for rectal administration. The euphoria from rectal administration is said to be similar to that from taking drugs orally, but it can help people avoid gastrointestinal adverse effects.
People who abuse oxycodone can get it on the street or from people who sell their prescriptions, but they can also go to a doctor and get it (i.e., going from doctor to doctor to obtain more than one prescription for oxycodone, all the while trying to avoid detection). They won’t need any accessories to swallow the oxycodone pills. However, there may be many prescription pill bottles from many doctors and pharmacies, all with dates that overlap.

Although it may seem self-evident, addiction is always a probable adverse consequence of oxycodone misuse. When a person takes a habit-forming drug, the body develops a tolerance to it. As a result, to achieve the usual desired high, a person must consume an increasing amount of the substance. Dependence grows as long as the use is continuous.
Withdrawal symptoms appear when someone stops using oxycodone or dramatically drops the usual dosage. Withdrawal symptoms can occur as soon as six hours after last use or as late as 30 hours after last use, depending on various circumstances, including the person’s duration and severity of oxycodone addiction. Symptoms may vary throughout the withdrawal process, but the following are examples of possible withdrawal symptoms:
It’s important to remember that opioid withdrawal can be dangerous due to complications from withdrawal symptoms like diarrhoea and vomiting, which can cause dehydration. As a result, it is strongly recommended that people seek help from a medical detox clinic or a drug rehab centre with a detox programme.
The severity of withdrawal symptoms can push a person to relapse and pose serious health risks. Individuals frequently relapse during withdrawal in an attempt to alleviate the severity of the symptoms.
No single cause or risk factor contributes to Oxycodone abuse. There are too many variables at play. Even so, there are patterns among opioid abusers. These patterns help understand some of the causes and risk factors. There are four leading causes of drug abuse and addiction:
In some people, the brain’s response to Oxycodone is such that the pleasurable feelings it causes are significantly stronger than they would otherwise experience. These strong emotions drive the user to use Oxycodone again, and again, and again. Some people’s brains respond to Oxycodone with a higher pleasure.
If a doctor initially recommends the drug for pain management, a person who already has a low pain threshold is in danger of becoming an Oxycodone abuser.
A person who tends to use narcotics recreationally is automatically in danger of abusing Oxycodone. Abuse can be defined as any usage of the drug for recreational purposes.
Some people may have a genetic susceptibility to addiction, according to research. However, this does not ensure that someone with this genetic propensity will become an addict. Oxycodone may not be the drug of choice among those who do.
There’s also evidence that those with a family history of drug misuse are more likely to abuse Oxycodone. Most crucially, people who have first-generation family members who have abused drugs (parents or siblings) are more likely to abuse drugs. This may be a taught behaviour rather than a genetic predisposition.
It’s important to keep in mind that the causes and risk factors frequently overlap. A family history of drug misuse, for example, is both a potential cause and a risk factor.
The high frequency of Oxycodone misuse and co-occurring diseases suggests that some people abuse the substance due to a mental illness. For example, someone suffering from severe depression may turn to Oxycodone misuse as a coping mechanism.

Because of its potential to induce sensations of euphoria, oxycodone is a stress-relieving medicine. As a result, those who cannot cope effectively with high levels of stress and anxiety are at risk of abusing Oxycodone after receiving a prescription.
The presence of side effects does not always indicate the presence of an addiction. When a person has an opioid use disorder, the larger the dose of opioids used, the more severe the adverse effects can be. A person who takes too much oxycodone, for example, may vomit if a side effect for a prescription user is nausea. Nonetheless, understanding the side effects of any opioid drug is beneficial because they provide a sense of what a person who abuses it may face.
The following are only a few of the possible side effects:
Abusing oxycodone might lead to convulsions or respiratory depression in certain people. Psychiatric disorders were reported by 1-5% of individuals in clinical studies. Even if it’s only a small percentage and the study didn’t focus on abuse, knowing the whole range of possibilities is useful. Other adverse consequences of abuse include:
People who abuse oxycodone run the risk of overdosing, which can be lethal. A partial list of overdose symptoms includes:
If you suspect someone is overdosing on oxycodone, call 999 immediately!
Mental health disorders are frequently associated with oxycodone addiction. This is referred to as co-morbidity or dual diagnosis. Co-occurring disorders include post-traumatic stress disorder (PTSD), bipolar disorder, and borderline personality disorder. The two most common co-occurring illnesses with oxycodone addiction are anxiety and depression.
Addiction is more likely to develop if you have a mental health problem. Both substance abuse and co-occurring disorders must be addressed during addiction treatment. Because the symptoms of addiction and other mental health issues overlap, this can be difficult. The underlying disease may go unnoticed if a person does not seek treatment until addiction has already set in.
Self-medicating can sometimes lead to addiction. Oxycodone and other medicines are used to alleviate feelings of guilt, shame, anxiety, and depression.
Self-medication is risky. The feeling of relief lasts only until the drug’s effects wear off. When someone is coming down after a high, depressive symptoms may be more acute. The worsening symptoms lead to more substance abuse, and the cycle continues indefinitely. When tolerance develops, and oxycodone no longer produces euphoria, people are in danger of suicide. Suicidal feelings are also a risk if you’re going through an unsupervised detox.
To be diagnosed with an opioid use disorder, at least 10 of these symptoms must be present throughout a 12-month period. The degree of a use disorder ranges from mild to severe on a scale of one to ten. The higher the number of symptoms present, the more severe the grade – usually six or more symptoms to be considered an addiction.
Physical, psychological, and behavioural elements are all covered by the 10 symptoms. As related to oxycodone, the following are paraphrased explanations of each of the 10 symptoms of an opioid use disorder:

People seeking treatment can obtain referrals from their health practitioners or contact drug treatment centres directly. The NHS offers a helpline to help patients locate the appropriate treatment services inside the NHS network. There are also several NGOs and private drug and alcohol treatment facilities available.
Questions regarding drug use, work, family, education, and housing circumstances are asked during the initial appointment. A urine or saliva sample is requested from patients. Throughout the rehabilitation process, key workers are accessible through the NHS to provide support and review treatment options and care plans. Talking therapy, medication-assisted treatment, medical detox to handle acute withdrawal, and support services are all addiction treatment options.
Call us on 0800 999 1083 for confidential help and to discuss your treatment options.
Buprenorphine-containing products include buprenorphine or a buprenorphine-naloxone combo. Both sorts are used to help people who are addicted to opioids. Subutex sublingual pills are an example of a product in this category, as are generic tablets or sublingual variants of Suxobone, Zubsolv, Bunavail, and Cassipa.
Don’t go through the process of recovery alone. Treatment providers can answer your questions. Get in touch with one today.
Call 0800 999 1083 today!
Buprenorphine is an opioid agonist and antagonist in one. It is commonly used in addiction treatment programmes to reduce withdrawal symptoms. Buprenorphine has a limit to its effects. It binds to opioid receptors in the brain but has only minor effects. Buprenorphine, unlike complete opioid agonists, reaches a point when its effects can no longer be increased.
Zubsolv is an opioid addiction treatment drug. It contains naloxone and buprenorphine. For 24 hours, one daily dose relieves withdrawal symptoms and reduces drug cravings. Sublingually is the most common method of administration.
Bunavail is a buccal film that contains buprenorphine and naloxone. It has a citrus flavour, and each dose comes in a yellow rectangle film. It’s applied to the inside of the mouth’s buccal lining or cheek lining.
Methadone is a prescription opioid that is manufactured in a lab. Methadone maintenance therapy, often known as tapering, is a successful treatment for opioid addiction and recovery. It lowers cravings while also providing pain relief. Methadone is a drug that can help people who are addicted to alcohol or drugs and are in pain. Methadone is a drug used in medication for pain reduction and a variety of other purposes.
CBT, or cognitive behavioural therapy, is a widely utilised treatment for substance abuse. CBT assists clients in identifying the ideas, feelings, and behaviours that lead to drug use. ‘Automatic negative thoughts are the triggers for drug use. CBT aims to assist patients in identifying and resolving automatic negative thoughts.
Individual therapy for substance addiction problems is usually part of a larger treatment plan. It focuses on the symptoms of depression, bipolar disorder, and other mental health illnesses, as well as helping clients deal with the ideas and situations that cause cravings. Individual counselling also assists individuals in understanding addiction as well as any co-occurring mental health conditions.
Family situations frequently influence addiction. The patient, as well as family members or close friends, participate in family counselling. Because addiction can affect multiple family members, family therapy provides support and coping techniques for everyone. Family therapy also aids non-addictive family members in comprehending what a loved one in treatment is going through.

In comparison to other drugs of abuse, tremendous progress has been made in the field of narcotics addiction treatment. Thousands of people have successfully overcome oxycodone addiction. Specific therapies, like medication-assisted therapy, are available to help people overcome opioid addiction. Pharmacological treatment alone will not ensure long-term recovery – it must be paired with counselling and support.
Contact your doctor or one of our addiction specialists to discuss treatment options for you or someone you know who is suffering from oxycodone addiction.

BACP accredited psychotherapist with 16 years experience working in mental health specialising in psychodynamic person-centred therapies treating those with a range of mental health disorders including anxiety, depression, OCD and Addiction.

Fill in your details and we’ll send you a message via SMS.

No matter where you live, there are drug and alcohol rehab options for you to discover. Treatment providers are waiting to answer your questions. Get started today.

Ever felt that gnawing ache or burning sensation in your gut after a night of drinks? You’re not alone. Stomach pain after drinking is a common complaint, and there are a few reasons why it might happen. Let’s delve into the science behind the discomfort and explore ways to soothe your stomach. The Irritating Truth: … Continued

Cocaine, a stimulant known for its short-lived burst of energy and euphoria, hides a dark side. Behind the initial high lies a dangerous potential for overdose, with severe health consequences and even death. This article delves into the world of cocaine overdose, equipping you with the knowledge to recognize the signs, understand the dangers, and … Continued

Adult smoking habits in the UK refer to how often and in what ways people aged 18 and above use tobacco. This includes everything from smoking cigarettes every day to occasionally lighting up, as well as using other tobacco products. Understanding these habits is important for several reasons: Public Health: Smoking causes many diseases that … Continued

Addiction in the UK is a complex issue that is connected to various aspects of society such as healthcare and law enforcement. It affects people from all backgrounds and has negative impacts on families, communities, and the entire nation. Understanding addiction involves not only looking at the uncontrollable use of substances and repetitive behaviors but … Continued

Don’t go through the process of recovery alone. Treatment providers can answer your questions. Get in touch with one today.
Call 0800 999 1083 today!








